Understanding Retinal Microvascular Changes in Systemic Lupus
The recent study on optical coherence tomography angiography (OCTA) in systemic lupus erythematosus (SLE) has opened up an engaging discussion on the early detection of ocular involvement among patients. This research not only highlights the power of noninvasive imaging but also underscores how closely our eyes and kidneys are interlinked in autoimmune disorders. As someone who has followed the evolution of diagnostic imaging for years, I find it both intriguing and promising that techniques like OCTA are beginning to carve a clear path through the tricky parts and tangled issues of early disease detection.
In this opinion editorial, we will take a closer look at this study and its implications, discuss the subtle parts of retinal microvascular change detection, and explore the role of OCTA as a key tool in managing SLE and lupus nephritis. Throughout our discussion, we will use everyday language that reflects the challenges of making sense of complicated pieces of data and the overwhelming nature of systemic illnesses. Let’s dive in and poke around the findings while keeping in mind the practical aspects for clinicians and patients alike.
Exploring the Role of OCTA in Early Detection of Microvascular Changes
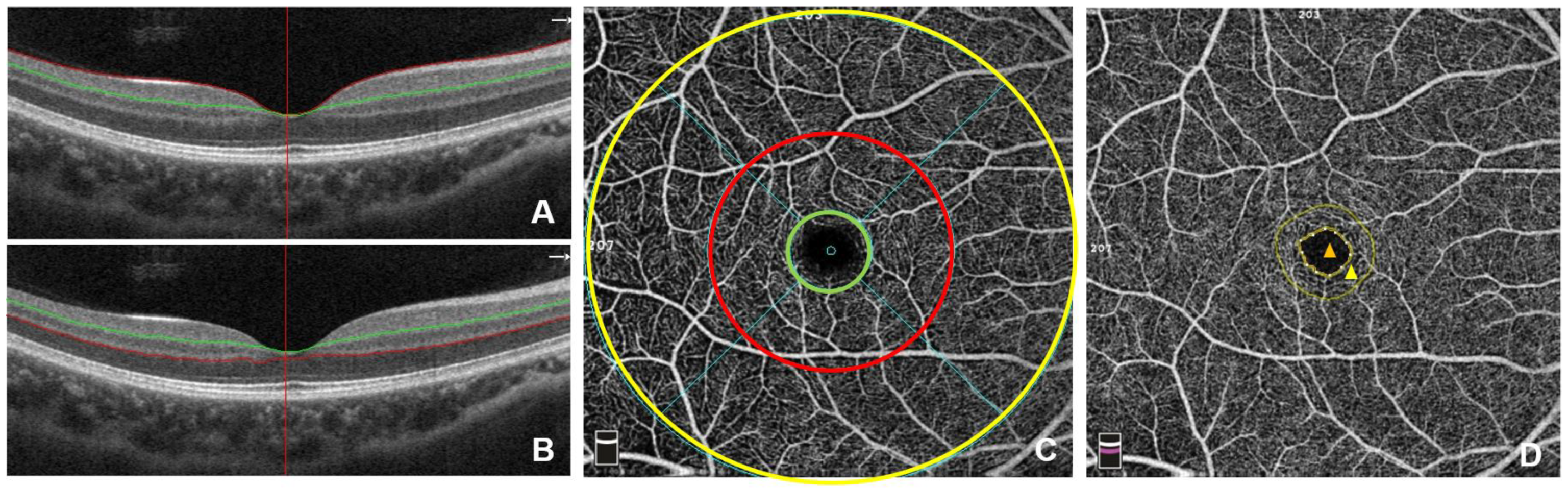
OCTA is emerging as a super important imaging technique that allows ophthalmologists to get into the nitty-gritty of the retinal microvasculature without resorting to invasive procedures. This tool provides high-resolution insights into the blood flow and structure of the retina, revealing fine details that could otherwise remain hidden. The study we are discussing has shown that OCTA can detect subtle changes in both the superficial and deep capillary plexus, even before patients develop overt retinopathy.
From an editorial perspective, the ability to catch these early warnings is like finding a tiny light at the end of a nerve-racking tunnel. In patients with systemic lupus, particularly those with lupus nephritis, these early signs include an increased foveal avascular zone (FAZ) and decreased vascular densities in both the superficial (SCP) and deep capillary plexus (DCP). These findings are a strong reminder that although the mechanisms behind these changes might seem loaded with issues, early recognition can help us steer through the maze of activation and progression in SLE.
Here are a few bullet points that neatly summarize how OCTA is revolutionizing our approach:
- Noninvasive imaging saves patients from the complications of invasive tests like kidney biopsies.
- Early detection of changes in retinal vascular density may serve as a proxy to monitor disease activity.
- Detailed imaging helps in identifying the subtle differences between patients with SLE and those with lupus nephritis.
- The method offers a path to customize immunosuppressive treatment to prevent further ocular damage.
The benefits of OCTA remind us that in the face of nerve-racking and intimidating clinical scenarios, modern technology can provide clinicians with a way to find their path in diagnosing and managing these conditions. It’s a promising tool that offers clear insights into the hidden complexities of lupus damage well before they become devastating.
Comparing Retinal Vascular Patterns in Lupus Nephritis and SLE
The similarities between eye and kidney involvement in SLE have been noted for years, yet the details often appear as tangled issues or confusing bits that are hard to articulate clearly. The study at hand has systematically compared patients with lupus nephritis to those with SLE without renal involvement, and the differences in retinal vascular patterns are both significant and enlightening.
For example, when comparing the central foveal thickness, both groups seemed similar. However, the FAZ area was significantly larger in patients with SLE – a detail that might at first glance be overlooked. More strikingly, the superficial capillary plexus (SCP) showed considerable reductions in vascular density, especially in patients with lupus nephritis. The SCP values read approximately 42.65% for SLE with nephritis, 44.88% for SLE without nephritis, and a healthy control group registered around 49.10%.
Similarly, the deep capillary plexus (DCP) exhibited even greater disparities. Here, not only were the overall values lower in the lupus nephritis group, but the margins in SLE without kidney involvement were only slightly better. In essence, the data suggests that while SLE in general affects the retina, those with nephritis are exposed to more intense twists and turns in the retinal microcirculation.
To organize these findings, consider the following table that outlines key metrics for both groups versus healthy controls:
| Parameter | SLE with Nephritis | SLE without Nephritis | Healthy Controls |
|---|---|---|---|
| SCP Overall Density | 42.65% ± 2.23% | 44.88% ± 2.09% | 49.10% ± 3.12% |
| SCP Parafoveal Density | 40.77% ± 3.27% | 47.19% ± 2.63% | 50.98% ± 4.80% |
| SCP Foveal Density | 18.96% ± 3.43% | 21.61% ± 4.00% | 24.16% ± 2.69% |
| DCP Overall Density | 48.04% ± 3.93% | 53.63% ± 2.19% | 54.88% ± 3.57% |
| DCP Parafoveal Density | 54.56% ± 2.37% | 56.93% ± 1.90% | 57.39% ± 5.99% |
| DCP Foveal Density | 34.42% ± 3.12% | 41.96% ± 3.19% | 42.55% ± 7.74% |
This comparative analysis is a powerful reminder that while the overall retinal thickness might not change drastically, the finer details – those subtle parts that define microvascular health – indeed do. Such slight differences can have a large impact on how we gauge the severity of SLE and specifically pinpoint the signs of lupus nephritis, urging us to take a closer look and act promptly.
Ocular Involvement as an Indicator of Systemic Activity
It has long been known that in systemic diseases like lupus, the eyes serve as a window to overall health. The research underpins the idea that even in the absence of manifest symptoms, small changes in the retinal microvasculature could indicate more widespread, systemic issues. In reading these findings, one can’t help but notice that the presence of retinal changes often signals active disease elsewhere in the body.
In fact, previous studies have suggested that nearly 88% of patients with visible retinal changes have active SLE. Such data is essential because it highlights how ocular examinations can sometimes flag potential systemic activity that might require urgent attention. The tracking of retinal vascular density and FAZ enlargement can therefore be used as a critical – or must-have – marker for disease monitoring in clinical practice.
On a personal note, this interconnectedness between the eyes and the rest of the body instills a sense of hope for early detection. If subtle changes in the retina, which are often easier to image and monitor over time, can alert clinicians to an impending systemic flare, we have an invaluable tool in our armamentarium. It opens up discussions on the need for interdisciplinary collaboration between rheumatologists and ophthalmologists, ensuring that patients who might otherwise be lost in the maze of symptoms are given proper attention early on.
Weighing the Advantages and Drawbacks of Noninvasive Imaging
OCTA represents a pivotal step forward in managing SLE and lupus nephritis, but like every diagnostic tool, it comes with its set of challenges and limitations. While it provides detailed imaging of the retinal vessels, the method is not without its confusing bits and intimidating factors. Operator expertise, image quality, and patient cooperation all play a role in ensuring accurate interpretation.
Let’s take a closer look at the pros and cons:
- Pros:
- Noninvasive approach – It avoids the nerve-racking risks associated with tissue biopsies.
- Early detection – Offers the ability to identify tangled changes before they become overtly problematic.
- Detailed analysis – Enables clinicians to measure various parameters, such as FAZ area and vascular densities, with precision.
- Enhanced monitoring – Facilitates regular follow-up examinations without subjecting patients to invasive examinations.
- Cons:
- Learning curve – The technique requires a familiarity with the hidden complexities of OCTA data interpretation.
- Image variability – Variability in imaging quality might make it challenging to compare sequential studies.
- Cost considerations – Although noninvasive, the advanced imaging equipment and expertise come at a significant cost.
- Limited scope – While effective for ocular microvasculature, OCTA does not provide a complete picture of overall systemic microcirculation.
In short, while OCTA offers essential insights with a noninvasive method, its use must be balanced with an awareness of its limitations. Clinicians should figure a path that integrates these imaging outcomes with other clinical findings to achieve a well-rounded approach to patient management.
Integrating Study Findings with Clinical Practice
The study’s findings provide a robust foundation for using OCTA as a guide in clinical decision-making. The distinct differences observed between patients with lupus nephritis and those with SLE alone suggest that ocular imaging could become a routine part of monitoring disease progression. It is important to note that while these differences might seem like mere twisting numbers to the untrained eye, they unravel the fine points that provide deep insight into systemic involvement.
For instance, the significant enlargement of the FAZ area in patients with SLE hints at an underlying deterioration in microvascular integrity. Coupled with the documented reductions in both SCP and DCP vascular densities, these objective measures give us a quantifiable handle on the situation. The clearer picture they offer is invaluable for timing the initiation or adjustment of immunosuppressive therapy.
From a practical standpoint, here are some suggestions for integrating these findings into clinical routines:
- Adopt regular OCTA screenings for patients diagnosed with SLE, especially those with a history of nephritis.
- Collaborate closely between rheumatology and ophthalmology departments to share insights and develop coordinated treatment plans.
- Use OCTA findings as a supplementary marker alongside traditional assessments such as kidney biopsies and serologic tests.
- Encourage ongoing training and development for imaging specialists to better interpret the subtle parts of OCTA data, ensuring consistency and accuracy.
These recommendations illustrate how, by making your way through the maze of diagnostic data, clinicians can tailor treatments early. The integration of imaging advances not only enriches our understanding of disease progression but also offers a lifeline to those facing the overwhelming burdens of systemic lupus.
The Impact of Retinal Microvascular Changes on Treatment Strategies
When it comes to treatment decisions for patients with SLE and lupus nephritis, timing and precision can make all the difference. The imaging revelations from OCTA provide us with critical information that can influence how immunosuppressive therapies are administered. Given that retinal changes can occur even before noticeable retinopathy develops, early intervention becomes a realistic and promising goal.
Recent evidence suggests that adjusting therapy based on such ocular findings may help in forestalling further retinal damage. For many clinicians, this represents a refreshing pivot from the traditional approach that often relied solely on systemic indicators. Instead, by focusing on the early twists and turns in retinal health, we’re starting to see how personalized treatment strategies can be built around noninvasive observations.
It’s worth noting that patients with lupus nephritis appear to be more susceptible to these ocular alterations. This means that they might need closer monitoring and potentially more aggressive treatment regimens. When thinking about the practicalities, consider this streamlined approach:
- Use OCTA imaging as an early warning system to identify changes before patients report visual symptoms.
- Review imaging results alongside other clinical markers to decide whether to intensify immunosuppressive therapy.
- Monitor the response to therapy by comparing sequential OCTA scans, ensuring that any further deterioration is caught promptly.
In many ways, this method is like having a dashboard for systemic lupus – one that helps clinicians figure a path through the confusing bits and monitor the delicate balance between disease activity and treatment efficacy. It is not only about reacting to overt manifestations of disease but also about anticipating future challenges and addressing them in a timely, proactive manner.
Patient Perspectives and the Real-World Impact of OCTA Findings
While the science and statistics surrounding OCTA and retinal microvascular changes are fascinating, we must always remember the human element behind the data. Patients who live with SLE face an intimidating array of challenges, from the nerve-racking prospect of kidney biopsies to the overwhelming uncertainty of visual health complications. OCTA offers a less invasive alternative that could alleviate some of these stresses.
From patient testimonials to clinical anecdotes, there is growing evidence that noninvasive imaging is making a practical difference in everyday lives. Many patients express relief at the possibility of routine eye examinations that provide a window into their overall disease state without the added anxiety of invasive tests. In discussions with healthcare professionals, it emerges that the clearer and earlier the diagnosis, the better the quality of life and treatment outcomes can be.
Furthermore, the incorporation of OCTA into the standard diagnostic toolkit is likely to promote more frequent and less stressful monitoring. As clinicians and patients work together to manage this complicated piece of a systemic illness, the priority remains clear: catching changes early to avoid the escalating costs—both emotional and physical—that come with delayed treatment.
Let’s summarize some of the key advantages these imaging techniques offer from a patient perspective:
- Reduced reliance on nerve-racking invasive procedures.
- More regular and accurate monitoring of disease progression.
- The possibility of adjusting treatment regimens before severe damage occurs.
- A greater sense of involvement in their own healthcare journey through easy-to-understand imaging results.
By reinforcing these benefits, the medical community can foster an environment where patients feel more in control, less overwhelmed by the twists and turns of their disease, and more optimistic about the future possibilities of personalized care.
Challenges and the Road Ahead for OCTA in Systemic Lupus Management
Despite the many advantages OCTA brings to the table, there remain a few challenging parts that need addressing as this technology becomes more widely integrated into routine care. One of the most complicated pieces is the prospect of ensuring that imaging centers are uniformly equipped and that clinicians working through the data are adequately trained.
There are several tangled issues that must be managed:
- Standardization of Protocols: Without a uniform standard for image acquisition and interpretation, the slight differences in assessment can lead to varied conclusions. This intensifies the need for collaborative frameworks and ongoing educational initiatives.
- Cost and Accessibility: As with many advanced diagnostic tools, the initial investment in high-quality OCTA machines can be off-putting for some practices, particularly those in less resource-rich settings. Over time, however, the benefits in early detection and treatment adjustment may well justify these expenses.
- Interpretation of Data: The hidden complexities in transforming OCTA data into actionable clinical decisions require that both ophthalmologists and rheumatologists work together. By finding their way through these subtle differences, interdisciplinary teams can help ensure that no critical detail is overlooked.
Looking ahead, it is clear that continued research, improved standardization, and cross-specialty collaboration will be essential. These steps will help refine the technology further and integrate it smoothly into the day-to-day management of SLE patients. The ultimate goal is to make this noninvasive method not just a supplementary diagnostic tool, but a definitive part of how we monitor and respond to systemic inflammation.
It is also worth noting that as further studies unfold, we may see even more refined ways to use OCTA data to predict disease flares or the onset of more severe complications. This proactive approach, rather than a reactive one, has the potential to reduce the overall disease burden significantly, both for individuals and the healthcare system at large.
Bridging the Gap Between Research and Routine Clinical Practice
Implementing OCTA in everyday clinical practice requires not only an appreciation of the subtleties observed in research studies but also a commitment to adapting our current healthcare infrastructure. There is a clear need to integrate these research findings into established protocols while ensuring that both the technical and human elements of healthcare are well aligned.
Clinicians must make their way through the maze of data by developing standardized checklists and continuing medical education sessions to bring everyone up to speed on the latest techniques. Some of the strategic approaches include:
- Interdisciplinary Training Workshops: Regular workshops for ophthalmologists, rheumatologists, and other relevant specialists can bridge the gap in understanding OCTA findings.
- Development of Clinical Guidelines: Establishing clear guidelines and reference values for retinal vascular densities in SLE can help streamline diagnostic and therapeutic decisions.
- Patient Education Programs: Informing patients about the benefits and limitations of OCTA can reduce anxiety, making routine monitoring a smoother process.
By taking these steps, the healthcare community can better address the somewhat intimidating aspects of transitioning new research into practical care. This collaborative approach, while it might seem like a nerve-racking task at first, is ultimately geared toward achieving more precise, personalized, and early interventions for patients with SLE.
Conclusion: Looking Forward in Lupus Management
In conclusion, the study on retinal microvascular changes in patients with systemic lupus erythematosus reminds us that even the smallest details can have a large impact on disease management. OCTA stands out as an influential tool that not only gets into the fine points and subtle parts of retinal imaging but also paves the way for a more nuanced approach to diagnosing and treating SLE and lupus nephritis.
While the data might appear daunting at first, with its confusing bits and nerve-racking twists, the practical benefits are clear. From early detection to informed treatment adjustments, OCTA offers hope that patients can avoid more invasive procedures and catch complications before they escalate. By taking a closer look at these early microvascular changes, clinicians have the opportunity to tailor immunosuppressive therapies more precisely, potentially preserving vision and slowing disease progression.
As we move forward, it is essential for healthcare professionals to continue collaborating and refining our understanding of these imaging techniques. Ongoing interdisciplinary training, standardized protocols, and consistent patient education will be key to transforming these research findings into everyday clinical practice. It may be a challenging journey filled with tricky parts and subtle distinctions, but the potential rewards—in improved patient outcomes and more personalized care—are well worth the effort.
Ultimately, the insights provided by OCTA in the context of SLE offer both a clearer view of ocular health and a glimpse into the broader picture of systemic disease activity. By embracing these new technologies and integrating them thoughtfully into our diagnostic pathways, we can ensure that every patient’s journey is marked by early intervention, personalized treatment, and a brighter, more hopeful future.
Originally Post From https://europe.ophthalmologytimes.com/view/retinal-microvascular-changes-in-patients-with-systemic-lupus-erythematosus-importance-of-octa
Read more about this topic at
Unlocking ocular biomarkers for early detection …
The ADDF’s Diagnostics Accelerator Authors New Paper …